Unfortunately, the impact that the coronavirus, COVID-19, may have on us, our community and the nation is unknown. Will travel restrictions increase? Will business and school closures become the norm? What impact will the virus have on our jobs, the economy and our daily life? The fact is we don’t know. But here’s what’s likely. It won’t just go away in a month or two. Instead, it will take time to understand the impact. Time to develop a vaccine and determine how we can prevent it in the future. It will force us to remain aware of our surroundings and be diligent in finding ways to minimize the virus’s spread. Meanwhile, here’s one thing we do know.
The same steps that we use to minimize our exposure to influenza and other viruses are also effective coronavirus infection prevention strategies.

The common cold comes from the same coronavirus that is subjecting us to COVID-19. And the two conditions that are most likely to cause this type of virus to spread are direct contact with contaminated surfaces and by inhaling the airborne virus after individuals sneeze or cough.
Whether you are a healthcare worker or in any other business, with a potential COVID-19 vaccine months away, conscientious handwashing is one of the most important coronavirus infection prevention techniques you can take.
Handwashing Reminders
But, isn’t it obvious that we should wash our hands regularly and especially if we have an illness or are around people who do? Obvious, maybe, but in practical application, not so much. A study conducted by Cambridge University found that handwashing compliance in the hospitals they studied was around 40%. Further, a 2008 study found that in the average household, 39% of the members rarely or never wash their hands after they sneeze. Clearly, handwashing compliance is a problem.
And although posted hand hygiene and handwashing signs won’t solve the problem, they have been proven to help. For example, a study published in the journal of Health Psychology, found posting the image of man's eyes over the sanitizer dispensers boosted hand hygiene compliance by 33%.
 In addition, Adam Grant, a noted psychological scientist at the Wharton School, University of Pennsylvania, found the most effective messages about hand hygiene highlight the consequences for other people. For example, he tested the impact of these two statements on posted signs:
In addition, Adam Grant, a noted psychological scientist at the Wharton School, University of Pennsylvania, found the most effective messages about hand hygiene highlight the consequences for other people. For example, he tested the impact of these two statements on posted signs:
- “Hand hygiene prevents you from catching diseases."
- ”Hand hygiene prevents patients from catching diseases.”
. . . the sign referencing patients was the winner. Keeping patients safe motivated healthcare professionals to wash their hands. In fact, it increased gel use by 33% per dispenser, and healthcare professionals were 10% more likely to wash their hands. Deploying these types of signs are helpful coronavirus infection prevention steps.
Maintaining Hand Hygiene Compliance Long Term
How do you keep hand hygiene top of mind for the long term? There are various steps that can help these reminders remain top of mind. For example,
- Change the location - when a ”wash hands” reminder remains in the same spot it starts to blend into its surroundings. Changing the location every two weeks will help maintain their impact.
- Change the message - although Grant’s research found the “helping patients” message had the greatest impact, altering the message is another way to get it noticed and inspire action.
- Change the look - adding different colors and designs helps to maintain awareness, much like placing the reminders in different spots.
 At a time when heightened concerns over the coronavirus require increased infection prevention strategies and compliance, steps like these can help.
At a time when heightened concerns over the coronavirus require increased infection prevention strategies and compliance, steps like these can help.
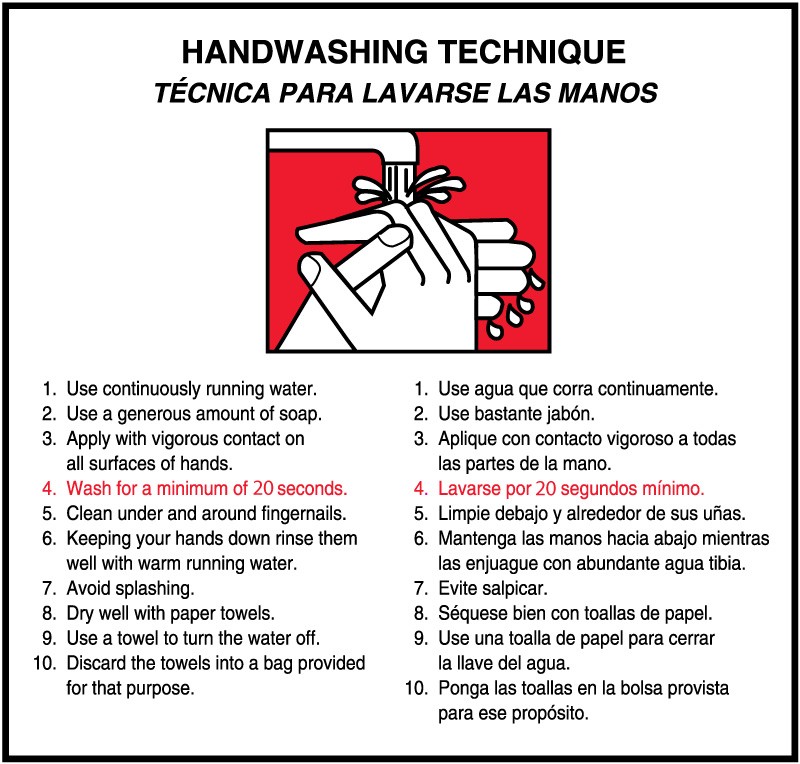
Hand Hygiene Instructions
But, once you increase compliance with handwashing, the job is not quite complete. A study from Michigan State University found that only about 5% of people actually wash their hands properly. In fact, providing instructions on how to effectively wash hands is another worthwhile endeavor. It’s useful to detail the appropriate steps.
Infection Prevention Techniques For Airline Travel
Lastly, if you or a patient’s plans call for air travel there are additional actions you should take. In addition to hand hygiene steps, take extra precautions with tray tables, airplane lavatories and aisle seats, all of which are germ magnets. Here are additional safeguards you should consider.
COVID-19 Patients
As of this current writing, more than 100,000 coronavirus cases have been identified worldwide, 1000 + in the United States. But as the number of patients suspected of contracting the virus increases, it requires extra attention from the staff and care teams.
Consider posting signs and posters at the entrance and in waiting areas, elevators and cafeterias to provide patients and visitors with instructions about hand hygiene, respiratory hygiene, and cough etiquette. And make sure you present the information in appropriate languages.
For care teams, if patients test positive, it’s essential to implement airborne precautions and strict contact precautions. Using proper PPE and contact precaution warning signs are essential protection steps. Plus, applying routing labels to medical record files for patients quarantined or in isolation guide crucial information with urgency and accuracy.
United Ad Label
United Ad Label stocks a complete line of Hand Hygiene and Infection Prevention products. In addition, the Custom Label Designer allows you to easily develop custom branded messages cost-effectively and with fast deliveries. Click here to learn more.
