When the national average gas price tops $5.00, it impacts every consumer that drives an internal combustion engine-powered car. And although the price at the pump dominates the headlines, the impact of oil prices that have nearly doubled in the last year affects far more than drivers. It impacts nearly all organizations including hospitals, ambulatory centers and physicians’ practices. In addition to shipping costs for parcels and less-than-truckload shipments increasing by 15% to 25%, input costs for items like antiseptics, personal protective equipment and IV tubing that are made from oil or natural gas have climbed as well. Mix in the recent COVID lockdowns in China, widespread staffing shortages and other supply chain disruptions and the result is higher costs for the supplies healthcare organizations use every day to run their operations. With inflation reaching the highest level since 1981, taking steps to combat those increases is especially important. How can healthcare organizations reduce the impact of inflation and rising costs?
How Inflation Impacts Health Systems
How much has inflation and rising costs impacted healthcare operations? The producer price index (PPI), which measures the average change over time in the prices domestic producers receive for their products, has increased 10.8% in the last year. For contractual agreements, the PPI is often used to calculate price changes so whether purchases occur from a previously negotiated contract or on an as-needed basis, costs have increased significantly.
Further, data from Kaufman Hall, a consulting firm that tracks hospital financial metrics, shows similar impacts with total hospital expenses up 11% compared to pre-pandemic levels in 2019. In addition, compared to 2019 levels, supply expenses for hospitals were up 15.9% through the end of 2021. When focusing on hospital departments involved most directly in care for COVID-19 patients − primarily hospital intensive care units (ICUs) and respiratory care departments − the increase in expenses is significantly higher.
Although pharmaceuticals and medical devices are typically the most significant expenditures for a healthcare organization, there are other cost centers that represent opportunities to mitigate costs.
How Can Healthcare Organizations Reduce the Impact of Inflation and Rising Costs?
In fact, medical supplies account for approximately 20% of total expenses. With input costs increasing, it’s difficult to imagine that the supplies healthcare organizations use will decrease in price anytime soon. But even as those costs increase, there are steps you can employ to lower the overall impact on your organization.
Improve Recurrent Healthcare Processes
Today, labor costs which include costs associated with recruiting and retaining employed staff, benefits and incentives, accounted for more than 50% of hospitals’ total expenses.
Further, according to the U.S. Bureau Of Labor Statistics, the average annual nursing salary is over $80,000.
In addition, with COVID burnout factors and other issues, the average turnover rate for nurses increased to 27.1%, an 8.4 percentage point jump from the 18.7% level in 2020. The annual wage costs multiply when a turnover occurs. For example, the 2021 NSI National Health Care Retention & RN Staffing Report determined the average cost of turnover for a bedside nurse averages $40,038 which causes hospitals to lose an average of nearly $5 million per year. Although the job challenges that nurses face make some turnover an occupational reality, streamlining processes can eliminate some of the nagging issues that contribute to job dissatisfaction.
Eliminating unnecessary challenges and ensuring the clinical staff remains as productive as possible is an effective cost reduction strategy.
Healthcare Labels Are Critical To Numerous Workflows
A poorly designed label that doesn’t work effectively for the specific application is like the home project that takes more time than necessary because you don’t have the right tools - with one exception, home projects don’t have patient safety implications.
IV Tubing
An estimated 90% of hospitalized patients in the U.S. receive IV therapy for medications and other fluids at some point during their stay. For line identification, medication type and dosage, the timing of tubing changes and more, labels are an essential part of the process.
An IV line label should include these essential data points. But, a lack of consistency in formats and the information contained on the label causes confusion among caregivers. Plus, with health systems employing floating, temporary and traveling nurses to meet staffing demands, consistency across departments and locations is paramount. Unfortunately, these types of inconsistencies lead to decreased productivity, job dissatisfaction and errors.
Cleaning and Disinfecting Medical Devices and Clinical Equipment
Cleaning these items typically involves water, detergents, chemical disinfectants or steam and pressure cleaning like an autoclave. And as important as cleaning regimens are to infection prevention and patient safety, they can create another problem - removing or obscuring important maintenance, calibration and safety information. When that occurs, the label no longer communicates essential calibration or safety information. Plus, a well-functioning device without the proper labeling can cause the medical staff to question the viability of the unit, forcing it offline, delaying treatment and creating unnecessary hassles.
Medical Storage Cabinets
Medical cabinets contain a small supply of essential items a nurse uses throughout their day including dressing trays, gowns, labels, linens, nasal prongs, pads, slider sheets, suction tubes and more. When supplies aren’t available in the nearby medical cabinet, nurses waste a significant amount of time walking to supply rooms. Avoiding unnecessary inventory expenses make sense, but not when key items are unavailable. Instead, it prevents clinicians from performing that task efficiently, adding unnecessary time and hassles to their rounds and ultimately increasing the overall health system costs.
Standardize Where Possible
A 200-bed acute care hospital uses, on average, 165 unique labels, typically a mix of stock and custom items. And, when you add in multiple facilities, clinics, physician practices, home health care and extended care facilities characteristic of many health systems, that number grows substantially. The dispersed locations, past purchasing practices and perceived unique product capabilities can lead to multiple vendors supplying common items.
Because the overall spend on labels is small compared to other supplies like PPE, bed linens and cleaning supplies, and don’t get the same priority in supply chain management, labels often fall into the “tail spend” category. Yet, targeting these purchases represents another area for potential cost savings.
Reduce Tail Spend
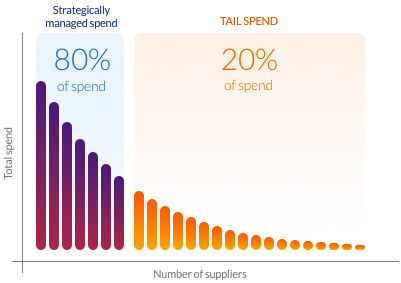
“Tail spend” is the perceived low-value spend that is often unmanaged or receives minimal procurement attention. Tail spend follows the 80/20 rule, typically representing 80% of transactions but only 20% of an organization's spend. These purchases normally take place outside of the supply chain/procurement operation and are often facilitated using p-cards.
Although it is prudent for organizations to prioritize high dollar value expenditures, not managing 20% of the budget can result in higher expenses than necessary.
 In fact, our research dating back over five years found that healthcare facilities typically use 7 to 15 different suppliers. And historically, the largest opportunity created by supplier consolidation is financial, in the form of lower costs. As the number of suppliers is reduced, buying power increases. Plus, fewer suppliers reduce the number of separate transactions, the amount of time it takes to manage those suppliers and more.
In fact, our research dating back over five years found that healthcare facilities typically use 7 to 15 different suppliers. And historically, the largest opportunity created by supplier consolidation is financial, in the form of lower costs. As the number of suppliers is reduced, buying power increases. Plus, fewer suppliers reduce the number of separate transactions, the amount of time it takes to manage those suppliers and more.
Although there are obvious benefits from vendor consolidation including cost savings and process cost reductions, it can also drive other positive outcomes. For example, using a variety of suppliers for key applications, like IV line and tubing labels, can contribute to product inconsistencies which add to the process inefficiencies noted above.
Focus on Healthcare-Associated Infections (HAIs)
Approximately 1 in every 31 patients in the United States has at least one HAI. And although the severity of the infection on patients differs, the average cost to the healthcare organization is approximately $25,000 per occurrence.
Standardizing environmental services can reduce the risk of HAIs and the overall costs of those services.
One infection control challenge is the difficulty in maintaining compliance. For example, a JAMA Internal Medicine research study found that hand hygiene compliance reached more than 90% in March 2020. Yet in just over a year, many healthcare workers regressed to previous habits.
There are various reasons for that regression to the mean. Workload is one factor. As nurses attend to a larger patient load or confront unexpected challenges, the common hand washing process they normally follow may be skipped in order to provide care. Also, even though caregivers understand the importance of infection prevention steps, it requires regular education and training to reinforce that message. Plus, with turnover increasing it’s particularly important to provide ongoing reminders.
Much like education and training, signage both reminds and instructs healthcare workers on the importance of taking hand hygiene steps and the appropriate methods to follow. Learn more about effective infection control steps you can take here.
United Ad Label
Although pricing pressures are likely to remain an issue over the near term, taking steps like those outlined above will have continued benefits today and once cost challenges diminish. In addition to supplying stock and custom healthcare labels, United Ad Label specializes in evaluating your operation to identify cost-saving opportunities. Contact us to learn more.


